In my albeit limited experience, I have found that one of the best remedies for my constant worry that something might go wrong, is when something actually does go wrong, and everything then turns out fine. While being a remarkably unpleasant experience at the time, it does however allow my brain to recalibrate, and to learn to accept that people can get sick, stuff can go awry, and it doesn’t always end in tears. This was one such occasion.
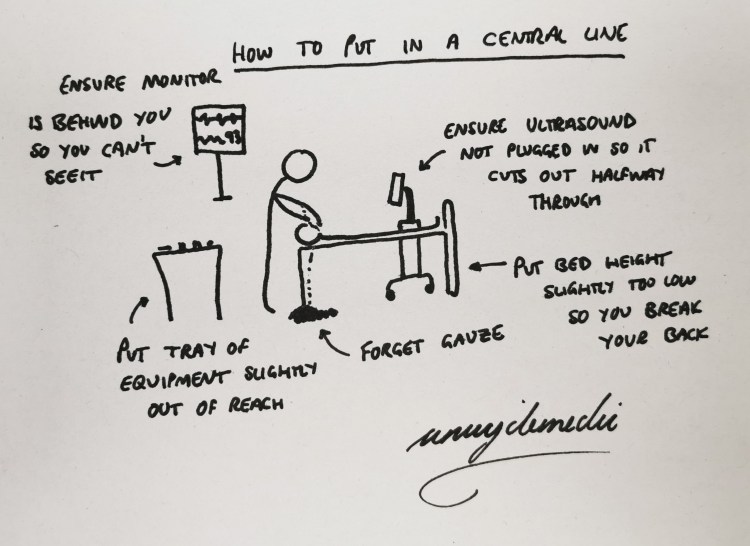
While working on the intensive care unit during the COVID-19 pandemic, I had been tasked with replacing a central venous line on a rather overweight lady whose previous central line had become dislodged and was no longer flushing properly into her femoral vein. By this stage I was a junior clinical fellow (F3) and moderately practised putting lines in, but was still fairly nervous around ventilated patients and especially those with COVID-19 who had apparently decided the traditional rules of ventilation didn’t apply to them and would desaturate spontaneously regardless of your input as a doctor.
I started by checking what this lady was being given through her central line, which was a combination of propofol (sedation), fentanyl (pain relief and to stop her cough reflex being triggered by the endotracheal tube) and noradrenaline (to keep her blood pressure up). All of these drugs would need to be continued while putting the new line in, as it takes long enough to do the procedure that she’d potentially start waking up, or her blood pressure would crash. So I put in a couple of cannulas so these infusions could be given peripherally, and the old central line could be taken out. (For the detail-oriented reader, the noradrenaline was swapped for metaraminol while being given peripherally, as norad tends to only be given via a central line.)
Having re-established the infusions, I checked that Justine, the patient’s ITU nurse, was happy for me to put a new line in and set about getting my equipment ready. I went through my usual double-triple checking of the needle, guidewire, dilator, line with all lumens flushed and clamped, scalpel, suture, dressing… all okay. I scrubbed up and prepped and draped the patient the same way as always, and made sure all my kit was in reach, the bed height was alright and monitoring was established. All good. Ready, set, go.
The first step is to find the vein using the ultrasound, which for the internal jugular where I was going is usually fairly straightforward. Then you adjust your probe position to centre the vein on the screen, and stick the introducer needle, loaded onto an empty syringe, into the skin right next to the middle of the ultrasound probe, hoping that it’s vaguely near the vein. Hopefully you can then see the needle on the ultrasound image and carefully guide it down into the vein while pulling back on the plunger, such that once you hit vein you get a satisfying flow of blood back into the syringe. Now you can breathe and put the ultrasound probe down.
Step 2 is to stabilise the needle with your non-dominant hand and twist the syringe off. Blood should dribble gently out of the end of the needle. It should not hit the ceiling. Assuming you’re not in the artery, you can then grab your guidewire and slide it down the needle into the vein.
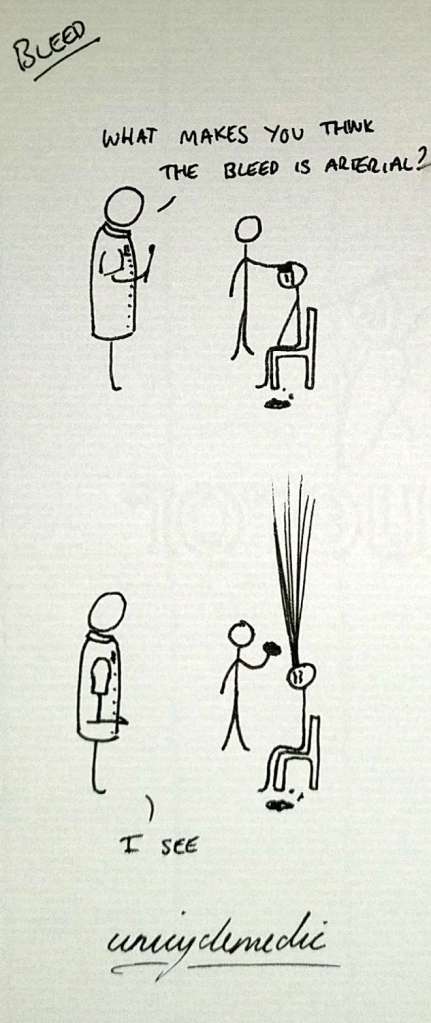
Pro tip: never force anything in medicine, especially guidewires.
Once your guidewire is a decent way in, you can take the needle out and slide it off the end of the wire, leaving the wire poking out the skin, making sure never to let go of the wire. At this point I like to pick up my ultrasound probe again and check that I can see the wire in the vein. Once you’re happy, make a small nick in the skin with the scalpel to open the hole a little more and then slide your dilator over the wire, and into the vein. This opens up the path through the soft tissue, which makes inserting the line easier. At this stage you might get a bit of blood coming up the dilator around the wire, which is a pretty reliable sign you’re still in the vein.
Normally the next step is to remove the dilator and insert the central line over the wire, however at this particular stage I was promptly informed by Justine that the patient wasn’t breathing, the ventilator wasn’t able to get any air in or out of the patient (who was presently buried under an enormous sterile drape) and that the patient’s oxygen saturations were dropping.
Well shit.
That all-too-familiar sensation of dread began to rear its head, crawling up my spine and filling my gloves with sweat. I hadn’t mentally prepared for exactly this scenario during one of my many midnight worry sessions, so obviously my eyes started blurring over and I instantly decided that I wanted to quit medicine right now and put my pyjamas on. But that sort of approach to acute emergencies is generally frowned upon in the ITU community so I had to think about doing something else instead. I looked up at the monitor which was currently a disco of red and yellow flashing lights telling me I wasn’t doing a very good job as a doctor.
Now seemed like a good idea to try that whole ‘not focusing on outcomes‘ thing and just work on what I should do next, which in medicine is invariably:
Reassess using an ABCDE approach…
I asked one of the other nurses to call the boss for help as I started assessing the airway and Justine checked the ventilator over. With the monitor and ventilator arguing over which of them was more distressed, I figured it would be a sensible plan to look at the tracheal tube first. I wasn’t airway trained so there wasn’t much I was going to be able to do about any problems that I found, but hey, I guess I could check that it was still vaguely in the right position. So I carefully lifted the drape, guidewire and bleeding dilator still in my other hand, to see if there were any clues. Sure enough my patient had decided, having not had much sedation since her previous central line stopped working, that having a large needle inserted into her neck was enough of a stimulus to counteract the propofol trickling into her cannula and had bitten down hard onto her tube, stopping any gas going in or out. Not good, but something I could sort and certainly better than a number of the other possibilities. Feeling all clever and proud of my diagnostic genius, I turned to the vastly experienced Justine to ask her to give a bolus of propofol, but she had already done it and the ventilator had stopped alarming.
At least I’d figured it out too I guess?
I’d somehow managed to keep my sterile field intact so I finished the procedure by sliding the line in and removing the wire, checking that the line was bleeding back and then flushed it and fixed it in place. I thanked Justine, told my boss to stand down and then went for a sit down and waited for my vision to normalise.
I chatted through the scenario with a colleague, who essentially gave the enlightening advice of:
“Yeah, it’s shit when that happens”.
While this wasn’t earth-shatteringly useful advice on how to manage the situation, it was a nice reminder that sometimes stuff just goes wrong regardless of what you have done to try and mitigate against it, and there’s nothing you can do other than respond appropriately. Often it’s a rapidly reversible problem and it provides a valuable learning experience. For me it was much more useful as an anxiety buster, because it allowed me to turn to my idiot brain and say,
“See!? We got this! Quit worrying so much!”
Stuff goes wrong, that’s understandable, and if you embrace the situation and reflect, it can provide a valuable learning experience. As long as you have made sensible decisions along the way, then you have nothing to fear.
